Understanding Psoriasis
A Comprehensive Guide for Patients
Introduction
Psoriasis is a chronic autoimmune skin condition that affects millions of people worldwide. If you have been referred to a Skin Consultant or are planning to visit one for the management of psoriasis, this comprehensive guide is designed to provide you with essential information about the condition, its causes, symptoms, treatment options, and lifestyle recommendations to help you better understand and manage psoriasis effectively.
What is Psoriasis?
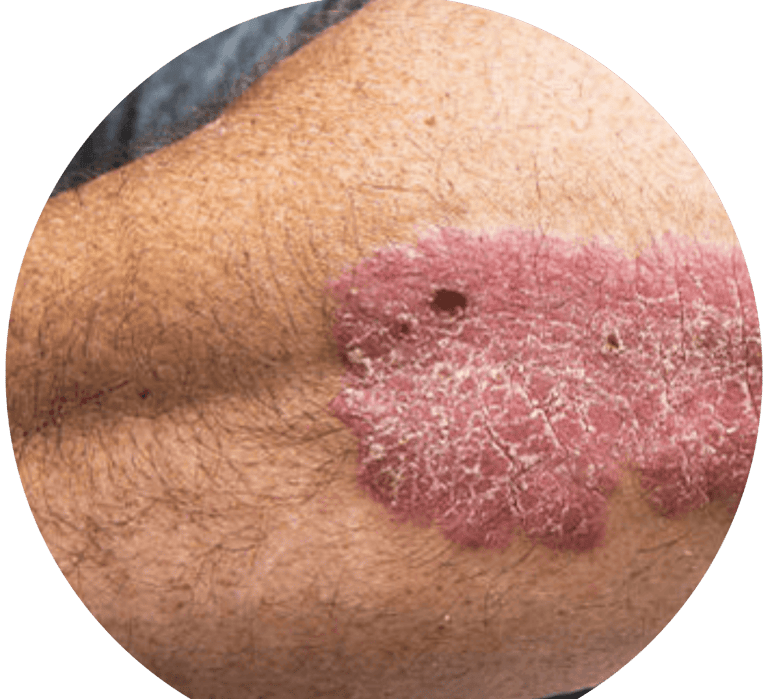
Psoriasis is a non-contagious skin disorder that accelerates the life cycle of skin cells, resulting in a buildup of thick, scaly patches on the skin's surface. It occurs when the immune system mistakenly attacks healthy skin cells, causing inflammation and abnormal skin cell growth. This leads to the formation of plaques, which can appear anywhere on the body, but are most commonly found on the elbows, knees, scalp, lower back, and nails
Symptoms of Psoriasis
The symptoms of psoriasis can vary from person to person, and the severity can range from mild to severe. Some common signs and symptoms include:
Red patches of skin with silvery scales
Dry, cracked skin that may bleed
Itching, burning, or soreness
Thickened, pitted, or ridged nails
Swollen and stiff joints (in some cases, psoriatic arthritis)
Causes and Triggers
The exact cause of psoriasis is not fully understood, but it is believed to be a combination of genetic and environmental factors. Certain triggers can exacerbate psoriasis symptoms, and these may vary among individuals. Common triggers include:
Stress and emotional factors
Infections, particularly streptococcal infections
Cold weather and dry air
Injuries to the skin, such as cuts or burns
Smoking and excessive alcohol consumption
Certain medications, like beta-blockers and lithium
Hormonal changes
Treatment Options
Psoriasis cannot be cured, but various treatment options are available to manage the symptoms and improve the quality of life for patients. The choice of treatment depends on the severity of the condition, the location of the plaques, and the patient's overall health. Common treatment options include:
Topical Treatments: These are creams, ointments, or lotions applied directly to the affected skin to reduce inflammation and scaling. They often contain corticosteroids, vitamin D analogs, retinoids, or salicylic acid.
Phototherapy: Also known as light therapy, this treatment involves exposing the skin to controlled amounts of natural or artificial ultraviolet light, which can slow the growth of affected skin cells.
Systemic Medications: For moderate to severe psoriasis, oral or injectable medications that work throughout the body may be prescribed. These include methotrexate, cyclosporine, and newer biologic therapies targeting specific immune pathways.
Combination Therapy: In some cases, a combination of treatments may be recommended to achieve better results.
Lifestyle Management: Lifestyle changes such as stress reduction, smoking cessation, and maintaining a healthy diet and weight can help manage psoriasis symptoms and improve overall well-being.
Contact
Reach out for appointments or questions
Phone
drchaubeypreeti@gmail.com
8853436234
© 2025. All rights reserved.
