Understanding Spider Veins
A Comprehensive Patient Guide
Introduction
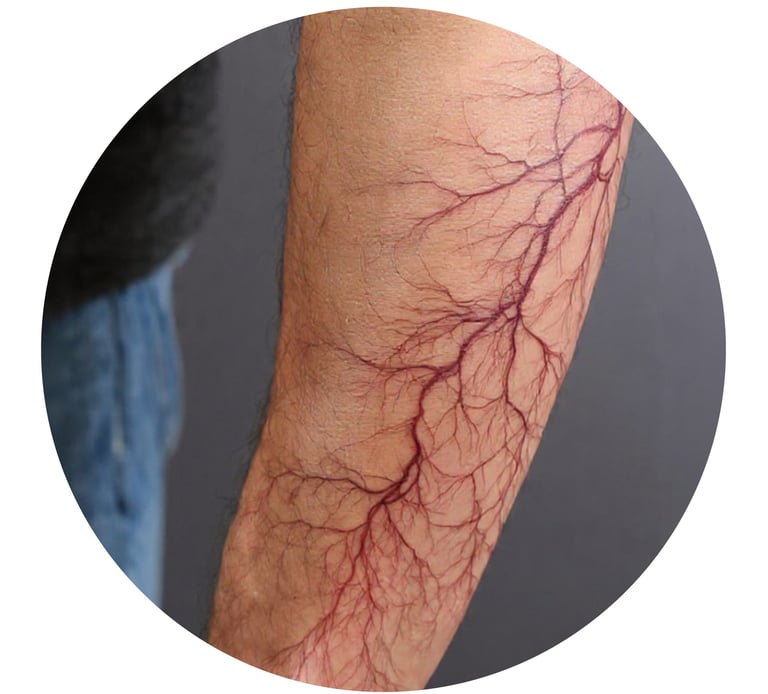
Spider veins, also known as telangiectasias, are small, thin blood vessels that appear close to the surface of the skin. They often form a web-like or tree branch pattern, hence the name "spider veins." While they are generally harmless, they can cause cosmetic concerns and, in some cases, discomfort or pain. This guide aims to provide comprehensive information for patients visiting a dermatologist to understand the causes, symptoms, risk factors, diagnosis, treatment options, and prevention of spider veins.
What are Spider Veins?
Spider veins are dilated capillaries that usually occur on the legs, face, and other areas of the body. They are more common in women than men and can develop at any age. These veins are red, blue, or purple in color and appear as fine lines or clusters on the skin's surface. Unlike varicose veins, spider veins do not protrude or bulge above the skin.
Causes and Risk Factors
Several factors contribute to the development of spider veins, including:
Genetics: A family history of spider veins can increase the likelihood of developing them.
Hormonal Changes: Hormonal fluctuations during puberty, pregnancy, menopause, or when using birth control pills can influence the development of spider veins.
Prolonged Standing or Sitting: Jobs or lifestyles that involve prolonged sitting or standing can strain the veins, leading to their appearance.
Age: As individuals age, the skin loses elasticity, and the veins become more visible.
Obesity: Being overweight can put additional pressure on the veins, causing them to dilate.
Sun Exposure: Excessive sun exposure can damage the skin and blood vessels, making spider veins more prominent.
Symptoms
In most cases, spider veins do not cause physical symptoms other than their appearance. However, some individuals may experience:
Itching or Burning Sensation: Spider veins may cause mild discomfort, such as itching or burning.
Leg Fatigue or Heaviness: When spider veins occur on the legs, some people may feel a sense of fatigue or heaviness.
Diagnosis
If you are concerned about spider veins, it is essential to visit a dermatologist or a qualified healthcare professional. The diagnosis typically involves:
Physical Examination: The dermatologist will examine the affected area to identify spider veins and assess their severity.
Medical History: Your healthcare provider will inquire about your family history, lifestyle habits, and any other relevant medical conditions.
Doppler Ultrasound: In some cases, a Doppler ultrasound may be performed to assess blood flow in the veins and rule out any underlying venous conditions.
Treatment Options
While spider veins are usually harmless, many patients seek treatment for cosmetic reasons. Several effective treatment options are available:
Sclerotherapy: This is the most common treatment for spider veins. A special solution is injected into the affected veins, causing them to collapse and fade over time.
Laser Therapy: Laser treatment uses focused light to target and break down the spider veins, gradually fading them away.
Intense Pulsed Light (IPL) Therapy: Similar to laser therapy, IPL uses intense light to heat and destroy the spider veins.
Vein Ablation: A minimally invasive procedure that uses heat or laser energy to close off and seal the affected veins.
Ambulatory Phlebectomy: For larger spider veins, a minor surgical procedure can be performed to physically remove the veins through tiny incisions.
Supportive Measures: Compression stockings can help improve blood flow and reduce discomfort associated with spider veins.
Contact
Reach out for appointments or questions
Phone
drchaubeypreeti@gmail.com
8853436234
© 2025. All rights reserved.
